Top stories in Newfoundland and Labrador
Local
MoreOpinion
MoreBusiness
MoreLifestyles
MoreSports
MoreCanada
MoreWorld
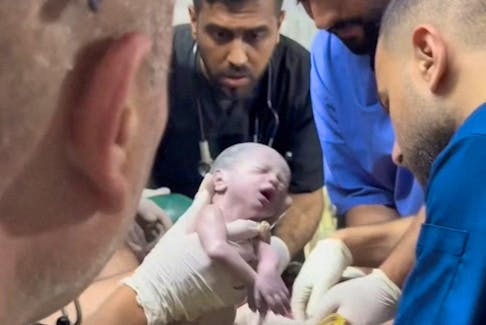
MoreGaza baby saved from dead mother's womb dies
By Mohammad Salem and Nidal al-Mughrabi RAFAH, Gaza (Reuters) - A baby girl who was delivered from her dying mother's womb in a Gaza hospital following an Israeli airstrike has herself died after just a few days of life, the doctor who was caring ...
Updated 13 minutes ago
|2 min read