“I feel great to be back at work doing what I’m good at, servicing our patients and the public and employing staff,” says Dr. Michael Connolly, a dentist with Belvedere Dental Clinic in Charlottetown, P.E.I.
Dentists in P.E.I. were among the first in Atlantic Canada to go back to work at the end of May after a mandated closure in March, but not without a lot of changes to the workplace and workflow practices.
Despite being a profession that works directly in patients’ mouths, Connolly says he is not nervous about being back to work. He says he feels safe using the new guidelines for the dental profession.
“The authors of these guidelines have worked hard in an environment where much more is unknown than known about the coronavirus,” he says.

Dr. Elizabeth Jackson, a dentist in Kentville, N.S., who recently started seeing patients in June, points out that dentists have always practiced strict infection control guidelines and personal protection. She believes the regulations for returning to work were well researched and thought out.
“We do have some new guidelines to follow to ensure our patients and staff continue to minimize the potential spread of infection, but I am confident that the new workflows are appropriate for all parties,” she says.
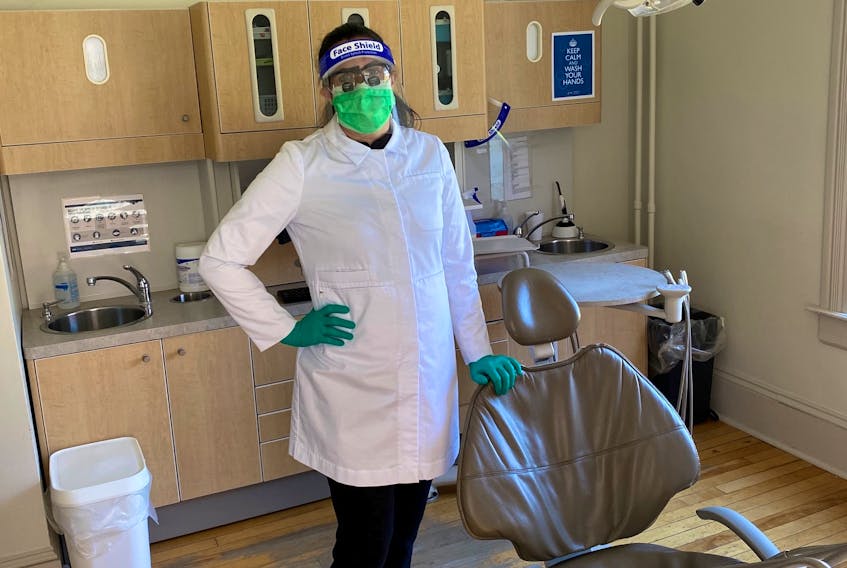
One of the first differences patients will notice is dentists’ new attire.
“We now have to wear a lab jacket or gown, and either wear goggles and a N95 mask, or a surgical mask with a face shield,” says Jackson. “We also now must wear scrubs and have dedicated clinic shoes. We will continue to wear gloves during appointments. And, we must wear a mask at all times while in the office when social distancing cannot be maintained.”
Dr. Linda Blakey, owner of Signature Dental in Mount Pearl, N.L., says her sister made the gowns for her office and she made the surgical caps. In addition, they had to install a washer and dryer.
“We must change into scrubs at the office, now, and no scrubs are to be worn outside,” says Blakey.
When it comes to other equipment, Jackson says there is still a shortage of masks, gloves, hand sanitizer, and gowns as dental suppliers must ration how much can be ordered weekly. All healthcare providers require similar supplies, so it makes ordering challenging, she says.
Despite the changes, Connolly says patients have been very accepting and understanding.
When asking patients about their experience at the dental office, Connolly says responses elicited included statements like, “I knew you’d look differently,” “I was prepared” or “I understood that you would be doing the right thing as professionals when you came back to work.”
Connolly says the responses were heartening, as it showed their patients trusted them to do the right thing, to be prepared and to provide a venue that was safe to be treated in.
But, he acknowledges, the new equipment can look a little intimidating for some people.
Jackson says she still hasn’t figured out a way to make the equipment look less scary. Now, she says, her patients will never see their dentist, hygienist or assistants without a mask on, and it can be hard to see though the layers of face protection.
To combat this, she is planning to make a video for her patients, to show them their faces before they get dressed in the personal protective equipment, and while they don their gear.
“I'm hoping if they can see each step, it won't look as intimidating,” she says. “I'm hoping the video will help show our new routine before they arrive.”
Physical distancing expectations
Not only are there these changes in attire, but physical changes had to be made to the workplace.
Before they reopened, Connolly says his staff had regular meetings over Zoom to keep them updated. They then brought staff back incrementally with an orientation.
“We needed to either place plexi glass at our front desk or have our receptionists wear masks (which would make it hard to talk on the phone),” explains Jackson.
“We purchased air purifiers for our operatories and our waiting room, removed all floor runners, pictures, extra stools in our operatories.”
The furniture in the waiting room was rearranged to accommodate social distancing guidelines.
The largest change has been to the workflow, says Jackson.
“We now need to personally speak to each patient before they arrive at the office to perform a COVID-19 screening. Once the patient arrives at the office, they call to let us know they have arrived,” says Jackson.
Basically, says Connolly, dentists are asking patients to use their car as a waiting room, as the front door of the office is locked.
Then, Jackson says, patients are met at the door, where they are given a mask if they don't have one, the screening questions are reviewed, and they must either wash their hands or use hand sanitizer.
In Blakey’s clinic, patients have their temperature taken as well as being asked a series of questions before they are brought to the operatory where they then rinse with a hydrogen peroxide pre-rinse before their procedure.
Once their treatment is complete, they replace their mask, sanitize their hands, see the receptionist and are escorted out another door to help maintain one-way flow of patients, says Jackson.
“The staff member that greets patients opens all doors for them, must sanitize the washroom after each use, and must sanitize all high-touch surfaces in between patients,” says Jackson.
“In our operatories, we always wiped all of our working surfaces in between each patient, but now must wipe everything in the room, including window frames.”
Aerosols must also settle for 15 minutes before disinfecting, which takes time, says Blakey.
As a result of these extra practices, the number of patients has decreased, says Blakey, who is now working 12-hour days to accommodate patients.
“My partner and I have increased the practice hours to see more patients and allow for physical distancing for patients,” she says.
This weird new world, says Blakey, has its challenges.
“It is the PPE we have to wear, it is the long days we have to work to make less income, it is the fact that we can’t give people toothbrushes to take home or kids their treats when they are being star patients,” Blakely adds.
And, as Connolly says, everything takes longer.
“I’m not complaining. If this is what’s necessary from a public health perspective, then I’m good with it,” he says.
All of these changes are expensive to implement. Many small businesses qualified for a federal small business loan to help with overhead costs during mandated closures, and in Nova Scotia, each dental office is eligible for up to $5,000 from the provincial government to help with the costs, says Jackson. Most of the cost, however, was absorbed by her clinic’s overhead costs, or may be made up with increased fees.
In the end, Blakey points out that dentists are also healthcare professionals but were not considered frontline.
“We wanted to be there for our patients. We followed emergency protocols to keep patients out of pain and out of emergency rooms. We have done what we can to help during this pandemic although the public healthcare system doesn’t seem to realize this. We will keep doing what we do and know we are helping in our own way,” says Blakey.
Throughout it all, Connolly says, patients are at the forefront.
“We support one another, and we do better everyday we come to work. We are there for the patients, because without patients, the lights would be off,” he says.