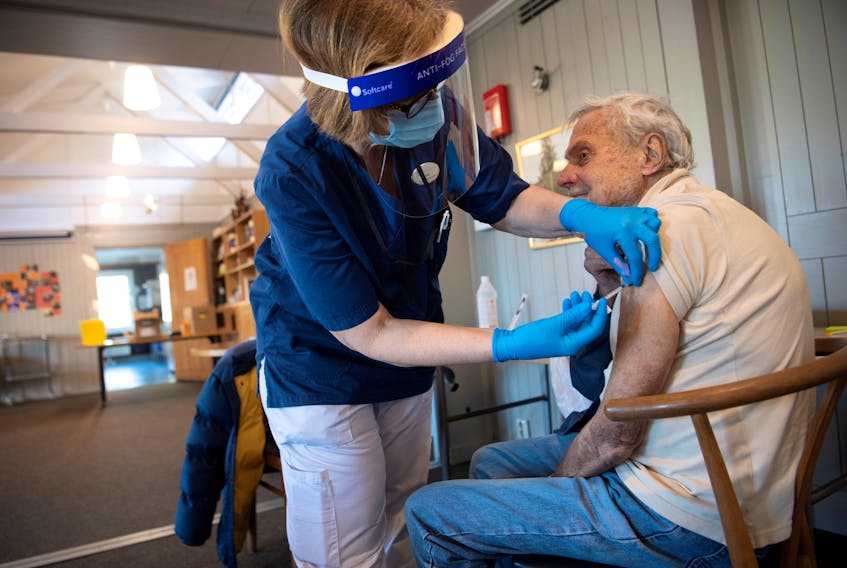
ST. JOHN'S, N.L. — While scientists debate the overall wisdom of extending the time between COVID-19 vaccine doses to four months, new data out of British Columbia suggests the practice may be even more dubious when it comes to seniors.
A joint team led by Simon Fraser University’s Dr. Mark Brockman published its initial non-peer-reviewed findings in the Canadian Medical Association Journal on March 24.

The group conducted antibody tests on seniors in long-term care over the past three months who have received their first dose of vaccine and compared them with a control group of health-care workers who were also vaccinated.
The seniors had a median age of 82.
They found the immune response in the older residents was, on average, four times less robust than in the control group.
“The question is, is their immune response enough to protect them, and for how long?” Dr. Marc Romney, one of the researchers who did serology testing out of the University of British Columbia, told The Telegram in a phone interview.
“A one-size-fits-all approach, with the four-month extension, may not necessarily be the best approach.”
The four-month window was recommended by the National Advisory Committee on Immunization (NACI) in early March. So far it has been adopted by B.C., Alberta, Quebec and Newfoundland and Labrador.
In this province, Chief Medical Officer of Health Dr. Janice Fitzgerald has said she takes her cues from the NACI, but remains open to change as new evidence emerges.
With a $1.2M @COVIDimmunityTF grant, FHS profs Zabrina Brumme & Mark Brockman are co-leading a study to examine the strength and durability of immune responses in residents and staff of long-term care facilities following #COVID19 vaccination.
— SFU Health Sciences (@SFU_FHS) March 1, 2021
Read more: https://t.co/UvciI0B435 pic.twitter.com/U1M6QxnqCi
Not as robust
Romney said the team has only looked at antibodies until now, but will also test for other parts of the immune system, such as T-cells, in the future. As well, they have not yet tested seniors living in the community.
“We looked at a critical piece of the immune response, which is antibodies, and we found that antibody levels in older people who live in long-term care were significantly lower after the first dose compared to health controls — about four times lower,” he said. “They were lower not only in magnitude, but their function was also not as robust.”
He said he understands the rationale for spacing out the doses, since many areas of Canada are poised to enter a third wave of the COVID-19 pandemic and variants of concern are starting to gain ground.
The B.1.1.7 variant, first detected in the U.K., was responsible for last month’s outbreak in the St. John’s region, and Romney said Vancouver is seeing a rise in cases of the P1 variant, the dominant strain in Brazil.
With limited vaccine supplies, Canadian health authorities are basically in a race to get at least one shot in as many arms as possible.
“I agree with extending the dosing interval for young people. It makes sense, immunologically,” said Romney.
“We just want to make sure that older people, vulnerable populations, aren’t left out of the equation with the extended dosing interval,” he said.
“Maybe the dosing interval shouldn’t be quite as long in those people because it’s going to leave them potentially vulnerable, especially when there are variants that are circulating, some of which can evade the immune system.”

NACI reviewing data
Funding for the B.C. study came from the national COVID-19 Immunity Task Force, which is directly connected to the NACI, so Romney says the committee would already be reviewing the results of the study, as well as similar studies taking place around the world.
On Thursday, Health Canada’s chief medical adviser, Dr. Supriya Sharma, confirmed that.
“There have been some studies to show there may be a bit more of a dropoff on immunity and protection after a certain point in time in certain groups, such as people that are elderly or have compromised immune systems,” she said.
But Romney, who credits Brockman and colleague Dr. Zabrina Brumme for most of the work on the study, sees a positive side to the research.
“The good news is we have some public health data showing that a single dose has had an incredible impact on decreasing hospitalizations and the number of outbreaks,” he said.
“The more information that you have, ultimately, the better decisions that you make.”
Peter Jackson is a Local Journalism Initiative reporter covering health for The Telegram.